Masseter-to-facial Nerve
Transfer

Masseter-to-facial nerve transfers are a treatment option for smile restoration when the main trunk of a patient's facial nerve is damaged or unavailable but the distal nerve branches and facial muscles remain viable. These techniques are best suited to cases of facial paralysis less than 2 years in duration. Adjacent functioning nerves can be divided and connected to the damaged facial nerve. Over time, the fibers from the donor nerve will repopulate the facial nerve and produce facial movement.
At Houston Methodist's Center for Facial Paralysis Surgery and Functional Restoration, the motor nerve branch to the masseter muscle has evolved into the donor nerve of choice for reinnervating the muscles of the cheeks (smile muscles) and lips.
A nerve branch to one of the chewing muscles (masseter muscle) is redirected to selected branches (buccal) of the facial nerve (masseter-to-facial nerve transfer). The surgery is performed through a limited facelift incision and frequently produces a strong, natural appearing smile without disturbing the individual’s ability to chew. Biting down is initially required to produce a smile. However, there is the potential for the smile to become effortless over time.
Technique
The procedure is performed through a small incision placed in the natural skin crease in front of the ear. The facial nerve is identified and electrical stimulation performed to verify the absence of any meaningful function. If no residual activity is found then the branches of the facial nerve to the lips and cheek muscles are isolated and prepared for later microsurgical connection.
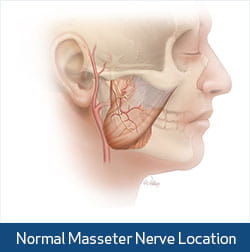
The motor nerve branch to a local chewing muscle (masseter) is explored. Once identified, the long branch of the nerve is freed from the muscle while the short branch is left intact. Preserving the short nerve branch helps maintain the muscle's function and natural size. Utilizing an operating microscope and sutures finer than a hair, a microsurgical connection is created between the facial nerve and masseter nerve.
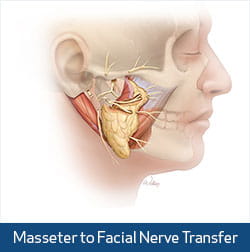
At that moment, the nerve regeneration process is set in motion. The nerve fibers from the masseter nerve will use the series of empty tunnels inside the damaged facial nerve to guide them to the muscles of facial expression. This process generally proceeds at a millimeter a day or an inch a month.
Following a masseter-to-facial nerve transfer, the majority of patients will have a single overnight stay in the hospital. In the post-operative period, patients are asked to avoid pressure to the affected cheek, exercise, heavy lifting and vigorous brushing of the teeth. A soft diet is usually prescribed for a period of two to three weeks. A home program of positive feedback exercises is also initiated.
The recovery of facial resting tone is usually apparent by the 5th post-operative month. Motion resembling the unaffected side often develops between the 6th and 7th post-operative months. Older individuals may require longer periods of time to achieve the desired function; however, the end result is usually comparable to younger individuals.
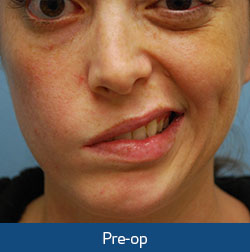
The strength and control over the reconstructed smile continues to improve over several years. Biting down will initially be required to produce a smile. Over time, however, the brain has the potential to undergo a re-education process (cerebral adaptation) resulting in the production of a naturally occurring, effortless smile.
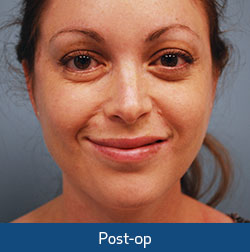
In addition to the potential for re-education, the masseter-to-facial nerve transfer has several extra advantages over other nerve donors. The nerve has a high density of motor axons and the ability to produce a strong smile with the proper orientation. The permanent difficulties with speech and swallowing associated with more traditional nerve transfers are also avoided utilizing this technique.
MASSETER TO FACIAL NERVE TRANSFER & CROSS FACE NERVE GRAFT
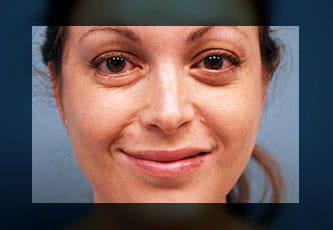
Surgical smile restoration by a Masseter to Facial nerve transfer and cross face nerve graft.
SMILE RESTORATION
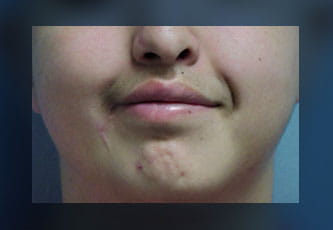
Smile restoration is one of the many procedures offered at Houston Methodist Center for Bells Palsy, Facial Paralysis Surgery & Functional Restoration.
real patient case studies
Learn how facial paralysis surgery and functional restoration can help you.
