Nerve transfers are indicated when the main trunk of the facial nerve is damaged or unavailable but the
distal nerve branches and
facial muscles remain viable. Adjacent functioning nerves can be divided and connected to the damaged facial nerve. Over time the fibers from the
donor nerve will repopulate the facial nerve and produce facial movement.
In the case of
cross face nerve grafts, the opposite undamaged facial nerve is utilized as a source of viable nerve fibers. A
dispensable sensory nerve (sural nerve) is usually harvested from the leg and utilized as a long interposition graft to connect the facial nerves on both sides of the face. The
cross face graft guides the regenerating nerve fibers as they migrate across the face to repopulate the injured muscles of facial expression.
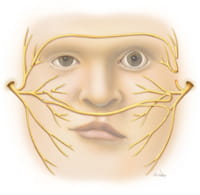
Once the healing process is complete, nerve signals will flow from the undamaged facial nerve across the graft into the previously paralyzed facial muscles producing movement. The nerve graft functions much like a telephone line delivering communication signals for the facial muscles. The ability to produce spontaneous, emotionally mediated movement is the greatest benefit of this technique.
Cross Face Nerve Graft Treatment
Before Surgery Video segment:
Complete left facial paralysis after excision of facial nerve schwannoma with loss of eye closure and protective blinking.
After Surgery Video Segment:
Here is the same patient 11 months after cross face nerve grafting to restore protective eye closure. Procedure performed by Dr. Michael Klebuc in Houston, TX.
The cross face nerve graft does have several limitations. The nerve regeneration process moves forward at the rate of approximately 1 mm/day or one inch per month. At this rate motion on the paralyzed side will not develop for 9 to 12 months. When the movement is restored it is usually weaker than the unaffected side.
In our reconstructive institute the cross face nerve graft is utilized primarily for reanimation of eye and brow. The technique appears most effective when utilized rapidly after the onset of facial paralysis/ Bells Palsy and is seldom employed as the primary reconstructive technique if the paralysis has been present for more than one year. In long standing cases of facial nerve paralysis (greater than two years) cross face nerve grafts can be utilized to power free muscle flaps.
Technique
The procedure is initiated by exploring the facial nerves on both sides of the face. This is performed through limited incisions placed in the natural skin crease directly in front of the ear. Electrical stimulation is utilized to verify the absence of motion on the damaged side and to map the function of individual facial nerve branches on the undamaged side.
As a general rule the human body has a surplus ability to perform any given function. For example we have two lungs and two kidneys although you can function with just one. This protective phenomena called functional reserve also exists in the facial nerve. There are usually several branches of the facial nerve that perform any given motion such as closing the eye, smiling or pursing the lips.
This functional overlap allows several branches to be divided and utilized for reconstructive purposes without impairing the normal function. After mapping the function of the facial nerve with electrical stimulation, several of the branches producing the desired motion are divided.
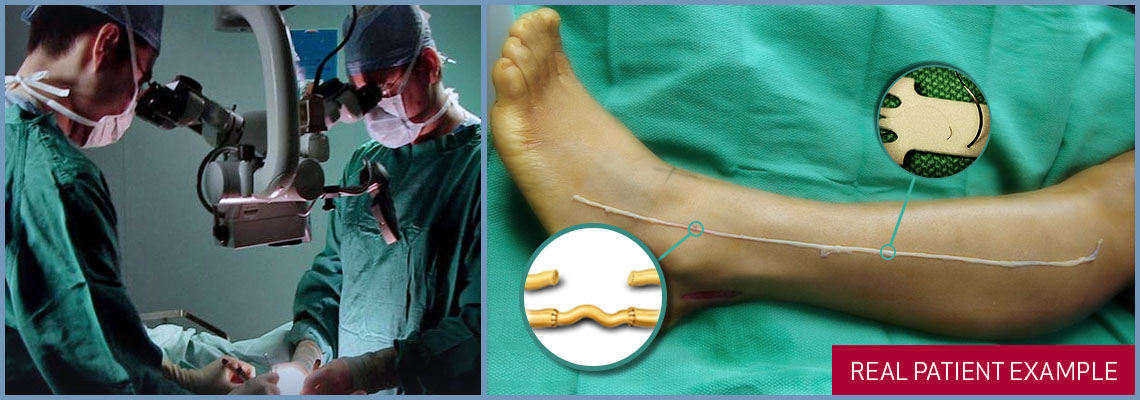
Attention is now focused on the leg where an expendable sensory nerve (sural nerve) is removed through a series of small incisions. A narrow tunnel is now created beneath the skin joining the two incisions in front of the ears. The nerve graft is passed through this tunnel and joined to the selected facial nerve branches with the aid of an operating microscope and stitches that are finer than a hair. After completion of the microsurgical nerve repairs the skin incisions are closed with absorbable sutures placed beneath the skin and a light bandage is applied.
Recovery
Typically a 24 to 48 hour hospital stay is required after this procedure. Ambulation is begun on the first post-operative day and a clear liquid diet is utilized for two to three days. In the early post-operative period patients are requested to stay on a soft diet and rinse their mouth after meals.
Exercise, heavy lifting, pressure to the cheeks and teeth brushing are all to be avoided until clearance is obtained from the operating surgeon. Harvesting of the nerve graft from the leg produces a region of numbness along the lateral ankle that is usually well tolerated and improves with time.
Return of facial tone and motion will usually develop between the 9th and 12th post-operative month. Electrical stimulation and a home physical therapy program are frequently initiated several months after surgery.
real patient case studies
Learn how facial paralysis surgery and functional restoration can help you.