Houston Methodist Experts Implant the Nation's First TriClip G4 for Tricuspid Regurgitation
June 2, 2021 - Katie McCallumOn April 26, 2021, heart experts at Houston Methodist became the first in the nation to perform a transcatheter tricuspid valve repair using a new clip-based technology called the TriClip™ G4.
The team, led by Dr. Stephen Little and Dr. Sachin Goel, is also the first in the world to implant this new device as part of the TRILUMINATE clinical trial, a global, multicenter study.
Through their participation in this trial, the Houston Methodist team aims to help bring a much-needed treatment alternative to patients suffering from tricuspid regurgitation — a historically understudied heart condition.
"The hope is that this trial and device will lead to a new, less-invasive approach for repairing a leaky tricuspid valve — often referred to as the 'forgotten heart valve,'" says Dr. Stephen Little, cardiologist and medical director of the Valve Clinic at Houston Methodist DeBakey Heart & Vascular Center.
Tricuspid regurgitation — a heart condition with few treatment options
Like many, Dr. Little has spent years frustrated by the lack of treatment options available to his patients suffering from tricuspid regurgitation — a heart condition in which the tricuspid valve does not close tightly enough, allowing blood to leak back into the upper-right chamber of the heart. Typically, this type of valve disease develops as a consequence of right-sided heart disease or pulmonary hypertension.
Currently, the only two FDA-approved modalities to treat a leaky tricuspid valve are medication therapy and open-heart surgery.
"Medication therapy works for some patients, but not all. When symptoms can't be controlled with medications, we look to surgery — but these patients are often so ill by that point that open-heart surgery is too risky," explains Dr. Little.
In fact, Dr. Little says that very few patients with advanced tricuspid regurgitation are candidates for open-heart surgery. Instead, medical therapy is commonly followed by palliative care.
"As a physician, it's very hard to have nothing left to offer your patient. What we've needed for quite some time is a way to repair a failing tricuspid valve without exposing our sickest patients to the risks of undergoing surgery," explains Dr. Little.
Expanding transcatheter repair techniques to the tricuspid valve
Using minimally invasive techniques to repair a failing heart valve isn't particularly new.
In fact, on the other side of the heart, transcatheter approaches have been used to repair the aortic and mitral valves for over a decade now — although experts are always refining and optimizing these techniques, as well as finding ways to extend them to more patients.
A transcatheter approach to repairing the tricuspid valve has lagged behind, however.
"We know that transcatheter valve repair can bring lower risk than open-heart surgery while still providing the same benefit in many cases. The question has been how to apply this approach to the tricuspid valve," says Dr. Little. "In the early stages of the TRILUMINATE trial, we investigated whether Abbott's mitral valve clip, MitraClip, could be used to repair the tricuspid valve as a last resort for patients with no other options."
But since the MitraClip is designed for the mitral valve, not the tricuspid, Dr. Little says it wasn't always a good fit.
"Still, you're always optimistic for new technology to come along. And when it finally does, you breathe a huge sigh of relief," adds Dr. Little.
For Dr. Little, relief came in the form of a new minimally invasive, clip-based valve repair system designed specifically for the tricuspid valve — Abbott's TriClip G4.
"Now that this technology is here, we're evaluating its benefit for patients with advanced tricuspid regurgitation who can't have surgery. Given the success we've seen in the past with other transcatheter valve repair approaches, we feel hopeful that the findings of this trial will be positive and make a difference," adds Dr. Dr. Sachin Goel, interventional cardiologist specializing in structural heart disease at Houston Methodist.
How the TriClip G4 works and is implanted
The TriClip G4 works by clipping the leaky tricuspid valve leaflets together, reducing the backflow of blood that contributes to symptoms of tricuspid regurgitation.
"The clip comes in four different sizes, giving us the ability to choose the size that works best for each patient's particular anatomy," says Dr. Goel.
Alongside the actual TriClip device comes a transcatheter delivery system uniquely created to maneuver to the tricuspid valve, as well as grasp the valve's leaflets and clip them together using the TriClip device.
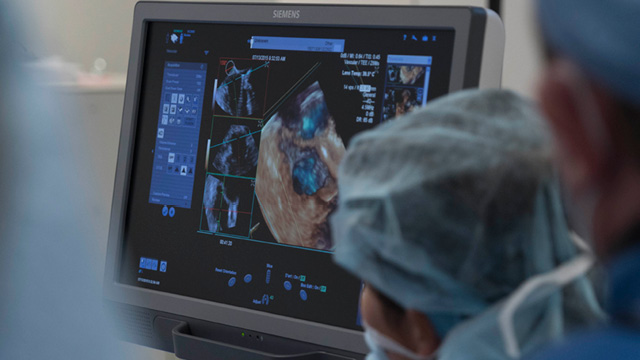
During the procedure, a catheter is inserted into the femoral vein of the patient's leg and steered through this vein to the right side of the heart. The TriClip is then implanted to fix the leaky tricuspid valve. All the while, transesophaegeal echocardiography (TEE) is used to visualize the heart and guide the procedure.
"The patient is under general anesthesia, but there's no heart-lung bypass, no sternotomy, no large incisions, no weeks of at-home recovery. Rather, there's one small incision in the leg and the patient goes home the next day with light bruising at the incision site," explains Dr. Goel. "This minimally invasive approach opens the door for us to repair a tricuspid valve in patients who are too high risk for surgery."
This new technology builds off of Abbott's MitraClip G4 for mitral valve repair, a system and technique Houston Methodist experts have been using to treat mitral valve disease for the last several years.
However, as with most things involving the heart and its intricate anatomy, this procedure isn't without its complexities.
A new challenge arises: How to best visualize "the forgotten valve"
Advanced imaging techniques are required to guide transcatheter procedures, something Dr. Little has extensive experience in. But, visualizing the tricuspid valve in this way is new — even to him.
"Before Abbott's TriClip technology existed, setting, optimizing and standardizing protocols for advanced visualization of this particular valve wasn't top of mind. It just hadn't been needed," explains Dr. Little. "Usually it's advancements in imaging that propels a minimally invasive approach forward, but, in the case of tricuspid valve repair, it was the TriClip technology that drove the interest in using advanced imaging to better visualize the tricuspid valve."
To make matters more complex, the tricuspid valve is inherently hard to see. Positioned in the anterior of the right side of the heart, its position doesn't make for easy viewing from the esophagus via TEE.
"It's the toughest imaging we're doing right now. We're essentially retraining ourselves, but we're also sharing this knowledge and what we learn with our colleagues around the country," says Dr. Little. "One of the most common questions I'm asked by my peers is, 'How are you imaging the tricuspid valve?'"
Next steps for transcatheter tricuspid valve repair
Right now, the TriClip G4 technology is only available in the U.S. through the TRILUMINATE clinical trial. The goal is for this TriClip system to become commercially available to patients with advanced tricuspid regurgitation in the coming years.
"We've been performing transcatheter aortic and mitral valve repairs for years, and experts at our institution played a role in the clinical trials that led to the approval of these devices and approaches. Now, we're leveraging that expertise to investigate the effectiveness of this new TriClip technology," explains Dr. Little. "We're expecting this approach will show benefit for patients with advanced tricuspid regurgitation — ultimately replacing surgery. Further down the line, it may even eventually show benefit earlier during disease course, too — possibly becoming an alternative to medication therapy."
Most importantly, Dr. Little says that this new technology provides him and his patients with hope.
"This is a field where we essentially had nothing, and now we have something. It still needs to be fully validated before it can become commercially available, but it certainly brings hope to patients who previously had very few options," adds Dr. Little.